
Life can be challenging: Build your own resilience plan

Nantucket, a beautiful, 14-mile-long island off the coast of Massachusetts, has a 40-point resiliency plan to help withstand the buffeting seas surrounding it as climate change takes a toll. Perhaps we can all benefit from creating individual resilience plans to help handle the big and small issues that erode our sense of well-being. But what is resilience and how do you cultivate it?
What is resilience?
Resilience is a psychological response that helps you adapt to life’s difficulties and seek a path forward through challenges.
“It’s a flexible mindset that helps you adapt, think critically, and stay focused on your values and what matters most,” says Luana Marques, an associate professor of psychiatry at Harvard Medical School.
While everyone has the ability to be resilient, your capacity for resilience can take a beating over time from chronic stress, perhaps from financial instability or staying in a job you dislike. The longer you’re in that situation, the harder it becomes to cope with it.
Fortunately, it’s possible to cultivate resilience. To do so, it helps to exercise resiliency skills as often as possible, even for minor stressors. Marques recommends the following strategies.
Shift your thoughts
In stressful situations, try to balance out your thoughts by adopting a broader perspective. “This will help you stop using the emotional part of your brain and start using the thinking part of your brain. For example, if you’re asking for a raise and your brain says you won’t get it, think about the things you’ve done in your job that are worthy of a raise. You’ll slow down the emotional response and shift your mindset from anxious to action,” Marques says.
Approach what you want
“When you’re anxious, stressed, or burned out, you tend to avoid things that make you uncomfortable. That can make you feel stuck,” Marques says. “What you need to do is get out of your comfort zone and take a step toward the thing you want, in spite of fear.”
For example: If you’re afraid of giving a presentation, create a PowerPoint and practice it with colleagues. If you’re having conflict at home, don’t walk away from your partner — schedule time to talk about what’s making you upset.
Align actions with your values
“Stress happens when your actions are not aligned with your values — the things that matter most to you or bring you joy. For example, you might feel stressed if you care most about your family but can’t be there for dinner, or care most about your health but drink a lot,” Marques says.
She suggests that you identify your top three values and make sure your daily actions align with them. If being with family is one of the three, make your time with them a priority — perhaps find a way to join them for a daily meal. If you get joy from a clean house, make daily tidying a priority.
Tips for success
Practice the shift, approach, and align strategies throughout the week. “One trick I use is looking at my calendar on Sunday and checking if my actions for the week are aligned with my values. If they aren’t, I try to change things around,” Marques says.
It’s also important to live as healthy a lifestyle as possible, which will help keep your brain functioning at its best.
Healthy lifestyle habits include:
- getting seven to nine hours of sleep per night
- following a healthy diet, such as a Mediterranean-style diet
- aiming for at least 150 minutes of moderate-intensity activities (such as brisk walking) each week — and adding on strength training at least twice a week
- if you drink alcohol, limiting yourself to no more than one drink per day for women and two drinks per day for men
- not smoking
- staying socially connected, whether in person, by phone or video calls, social media, or even text messages.
Need resilience training?
Even the best athletes have coaches, and you might benefit from resilience training.
Consider taking an online course, such as this one developed by Luana Marques. Or maybe turn to a therapist online or in person for help. Look for someone who specializes in cognitive behavioral therapy, which guides you to redirect negative thoughts to positive or productive ones.
Just don’t put off building resilience. Practicing as you face day-to-day stresses will help you learn skills to help navigate when dark clouds roll in and seas get rough.
About the Author

Heidi Godman, Executive Editor, Harvard Health Letter
Heidi Godman is the executive editor of the Harvard Health Letter. Before coming to the Health Letter, she was an award-winning television news anchor and medical reporter for 25 years. Heidi was named a journalism fellow … See Full Bio View all posts by Heidi Godman
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD

Orienteering: Great exercise and better thinking skills?

Picture this: you’re with friends in an unfamiliar forest using only a map and a compass to guide you to an upcoming checkpoint. There are no cell phones or GPS gadgets to help, just good old brainpower fueled by a sense of adventure as you wind through leafy trees and dappled sunlight.
This is not an excursion to a campsite or a treasure hunt. It’s a navigation sport called orienteering — a fun way to get outside, exercise, and maybe even help fight cognitive decline, according to a 2023 study.
What is orienteering?
Orienteering combines map and compass reading with exercise. Competitors (“orienteers”) race against a clock to reach checkpoints in outdoor settings that can range from city parks to remote areas with mountains, lakes, rivers, or snowy fields.
“You can go out in a group or on your own. You get a very detailed map and navigate your way to checkpoints that record your time electronically,” says Clinton Morse, national communications manager with Orienteering USA, the national governing body for the sport in the United States.
Because orienteers are racing the clock, they might run on trails, hike up hills, or scramble around boulders. That’s for foot-orienteering events. There are also orienteering events with courses geared for mountain biking, cross-country skiing, or canoeing.
How might orienteering affect thinking skills?
A small 2023 study published online in PLoS One found a potential link between orienteering and sharp thinking skills.
Researchers asked 158 healthy people, ages 18 to 87, about their health, activities, navigation abilities, and memory. About half of the participants had varying levels of orienteering experience. The other participants were physically active but weren’t orienteers.
Compared with study participants who didn’t engage in orienteering, those who were orienteers reported
- having better navigational processing skills (recognizing where objects were, and where participants were in relation to the objects)
- having better navigational memory skills (recalling routes and landmarks).
The study was observational — that is, not a true experiment — and thus didn’t prove that orienteering boosted people’s thinking skills. But the link might be plausible.
“Aerobic exercise releases chemicals in the brain that foster the growth of new brain cells. And when you use a map and connect it to landmarks, you stimulate growth between brain cells,” says Dr. Andrew Budson, lecturer in neurology at Harvard Medical School and chief of cognitive and behavioral neurology at VA Boston Healthcare System.
Where can you find orienteering opportunities?
There are about 70 orienteering clubs across the United States, and many more around the world (the sport is extremely popular in Europe). To find an orienteering event in your area, use the club finder tool offered by Orienteering USA.
How can you get started with orienteering?
People of all ages and athletic levels can take part, because orienteering courses vary from local parks to wilderness experiences. Costs are about $7 to $10 per person for local events, or $25 to $40 per person for national events, plus any travel and lodging expenses.
To make orienteering easy at first, Morse suggests going with a group and taking things slowly on a short novice course. “You don’t have to race,” he says. “Some people do this recreationally to enjoy the challenge of completing a course at their own pace.”
The trickiest part is learning to read the map. Morse’s advice:
- Turn the map as you change directions. Hold the map so that the direction you’re heading in is at the top of the page. For example, if the compass indicates that you’re heading south, turn the map upside down, so the south part is on top and easier to follow.
- Create a mental image of what the map is telling you. If there’s a fence along a field on the map, build a picture of it in your mind so you can recognize it when you see it, even if you haven’t been there before.
Tips for safe and enjoyable orienteering events:
- Dress appropriately. Wear comfortable clothes including long pants, good walking shoes, and a hat.
- Lather up. You’ll be outside for at least an hour, and you’ll need sunblock and possibly tick and bug spray depending on the terrain. Preventing tick bites that can lead to Lyme disease and other tick-borne illnesses is important in many locations.
- Bring some essentials. Pack water, a snack, sunblock, bug spray, and your phone. (Keep the phone turned off unless you need to call for help.)
- Use good judgment. Know that the shortest route on the map won’t always be the best, since it might take you up a hill or through thick vegetation. It might be better to go around those areas.
Once you learn the basics of orienteering, you can make it more physically challenging (and a better workout) by going faster and trying to beat your previous times, or by signing up for a more advanced course that’s longer and requires more exertion and speed.
And no matter which event you take part in, enjoy the adventure. “You’re not just following a path, you’re solving puzzles while being immersed in nature,” Morse says. “It’s a great way to experience the outdoors.”
About the Author

Heidi Godman, Executive Editor, Harvard Health Letter
Heidi Godman is the executive editor of the Harvard Health Letter. Before coming to the Health Letter, she was an award-winning television news anchor and medical reporter for 25 years. Heidi was named a journalism fellow … See Full Bio View all posts by Heidi Godman
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD

What is cognitive behavioral therapy?

Cognitive behavioral therapy (CBT) teaches people to challenge negative thought patterns and turn less often to unhelpful behaviors. These strategies can improve your mood and the way you respond to challenging situations: a flat tire, looming deadlines, family life ups and downs.
Yet there’s much more depth and nuance to this well-researched form of psychotherapy. It has proven effective for treating anxiety, depression, and other mental health conditions. Tailored versions of CBT can also help people cope with insomnia, chronic pain, and other nonpsychiatric conditions. And it can help in managing difficult life experiences, such as divorce or relationship problems.
What are the key components of CBT?
One important aspect of CBT relates to perspective, says psychologist Jennifer Burbridge, assistant director of the Cognitive Behavioral Therapy Program at Harvard-affiliated Massachusetts General Hospital.
“Therapists who practice CBT don’t see the problems or symptoms people describe as having one single cause, but rather as a combination of underlying causes,” she says. These include
- biological or genetic factors
- psychological issues (your thoughts, physical sensations, and behaviors)
- social factors (your environment and relationships).
Each of these factors contributes to — and helps maintain — the troublesome issues that might prompt you to seek therapy, she explains.
How does CBT describe our emotions?
Our emotions have three components: thoughts, physical sensations, and behaviors.
“Thoughts are what we say to ourselves, or 'self-talk,'” says Burbridge. Physical sensations are what we observe in our bodies when we experience an emotional situation: for example, when your heart rate rises in stressful circumstances. Behaviors are simply the things you do — or do not do. For instance, anxiety might prevent you from attending a social event.
All three components are interrelated and influence one another. That’s why CBT helps people to develop skills in each of them. “Think of it as a wellness class for your emotional health,” says Burbridge.
How long does CBT last?
CBT is a goal-oriented, short-term therapy. Typically it involves weekly, 50-minute sessions over 12 to 16 weeks. Intensive CBT may condense this schedule into sessions every weekday over one to three weeks.
Is CBT collaborative?
“When I first meet with someone, I’ll listen to what’s going on with them and start thinking about different strategies they might try,” Burbridge says. But CBT is a collaborative process that involves homework on the patient’s part.
What might that mean for you? Often, a first assignment involves self-monitoring, noting whether there are certain things, events, or times of day that trigger your symptoms. Future sessions focus on fine-tuning approaches to elicit helpful, adaptive self-talk, and problem-solving any obstacles that might prevent progress.
Certain thinking patterns are often associated with anxiety or depression, says Burbridge. Therapists help people recognize these patterns and then work with patients to find broader, more flexible ways to cope with difficult situations.
“We’re cognitive creatures with big frontal lobes that help us analyze situations and solve problems. That’s useful in some situations. But at other times, when you’re trying to manage your emotions, it may be better to pause and acknowledge and accept your discomfort,” says Burbridge.
Which CBT tools and strategies can help?
That particular skill — paying attention in the present moment without judgement, or mindfulness — is a common CBT tool. Another strategy that’s helpful for anxiety, known as exposure or desensitization, involves facing your fears directly.
“People avoid things that make them nervous or scared, which reinforces the fear,” says Burbridge. With small steps, you gradually expose yourself to the scary situation. Each step provides learning opportunities — for example, maybe you realize that the situation wasn’t as scary as you though it would be.
By trying new things instead of avoiding them, you begin to change your thought patterns. These more adaptive thinking patterns then make it more likely you will try new or challenging experiences in the future, thereby increasing your self-confidence.
How does CBT work?
Brain imaging research suggests conditions like depression or anxiety change patterns of activity in certain parts of the brain. One way CBT may help address this is by modifying nerve pathways involved in fear responses, or by establishing new connections between key parts of the brain.
A 2022 review focused on 13 brain imaging studies of people treated with CBT. The analysis suggested CBT may alter activity in the prefrontal cortex (often called the “personality center”) and the precuneus (which is involved in memory, integrating perceptions of the environment, mental imagery, and pain response).
Who might benefit from CBT?
CBT is appropriate for people of all different ages. This can range from children as young as 3 years — in tandem with parents or caregivers — to octogenarians. In addition to treating anxiety and depression, CBT is also effective for
- eating disorders
- substance abuse
- personality disorders
- attention deficit hyperactivity disorder (ADHD)
- obsessive compulsive disorder (OCD).
Additional evidence shows CBT may help people with different health issues, including irritable bowel syndrome, chronic fatigue syndrome, fibromyalgia, insomnia, migraines, and other chronic pain conditions. The therapy may also benefit people with cancer, epilepsy, HIV, diabetes, and heart disease.
“Many medical conditions can limit your activities. CBT can help you adjust to your diagnosis, cope with the new challenges, and still live a meaningful life, despite the limitations,” says Burbridge.
About the Author

Julie Corliss, Executive Editor, Harvard Heart Letter
Julie Corliss is the executive editor of the Harvard Heart Letter. Before working at Harvard, she was a medical writer and editor at HealthNews, a consumer newsletter affiliated with The New England Journal of Medicine. She … See Full Bio View all posts by Julie Corliss
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD
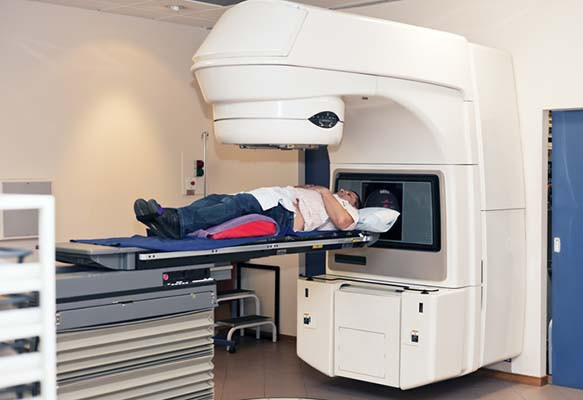
Prostate cancer: Brachytherapy linked to long-term risk of secondary malignancies

When cancer patients are treated with radiation, it’s possible that the therapy itself may cause new tumors to form in the body later. Radiation kills cancer cells by damaging their DNA, but if the treatments cause genetic damage to normal cells near the radiation target, there’s a small risk that these secondary malignancies may arise over time.
Just over 10 years ago, Canadian researchers set out to assess the risk of secondary malignancy among men with prostate cancer who were treated with a type of radiation called brachytherapy. Unlike radiation delivered from sources outside the body, brachytherapy is accomplished by implanting dozens of radioactive pellets, or “seeds,” directly into the tumor site. Those seeds, which are never removed, emit radiation at a dose that declines toward zero over the course of a year.
Brachytherapy has the advantage of convenience. Instead of traveling for repeat sessions of radiation, men need only one treatment, usually given in an outpatient setting. But brachytherapy is also falling out of favor, in part because newer types of external beam radiation deliver high-precision doses with fewer side effects.
Study methodology and results
The Canadian study compared rates of secondary malignancies in the pelvis among men treated either with brachytherapy or with surgery to remove the prostate. All the treatments took place in British Columbia between 1998 and 2000. The brachytherapy group included 2,418 men with an average age of 66, while the surgically-treated group contained 4,015 men whose average age was 62. Within that group, 2,643 men had been treated with surgery alone, and 1,372 men with surgery plus external beam radiation given later.
After median follow-ups of between 5.8 years (brachytherapy) and 6.4 years (surgery), the study team reported in 2014 that there was no difference in rates of secondary malignancies between the groups, or with cancer incidence in the general population.
But that’s no longer the case: In April 2024, the researchers published updated findings. This time, rates of new cancers in the pelvis — including the bladder and rectum — were higher in the brachytherapy group. Specifically, 6.4% of brachytherapy-treated men had secondary malignancies at 15 years of follow-up, increasing to 9.8% after 20 years. By contrast, 3.2% and 4.2% of surgically-treated men developed secondary pelvic malignancies over the same durations. There was no difference in deaths from secondary malignancies between the groups.
The strength of the association with bladder cancer in particular is “similar to that seen with smoking,” wrote the author of an accompanying editorial. Results from the study “should be considered when treating men with localized prostate cancer who have a long life expectancy,” the authors concluded.
Commentary from experts
“I do believe that this study reveals a dark truth about radiation for prostate cancer that has been long suspected,” says Dr. Anthony Zietman, a professor of radiation oncology at Harvard Medical School and Massachusetts General Hospital, and a member of the advisory and editorial board for the Harvard Medical School Guide to Prostate Diseases. “As the decades pass after radiation therapy of any kind — brachytherapy or external beam — the risk for radiation-induced malignancies rises.
“These malignancies are usually in adjacent organs like the bladder and rectum, or within the prostate itself. They may be very curable, and thus the survival rates are the same for radiation or surgically treated patients, but there is little doubt that, for these patients, they represent a ‘sting in the tail’ long after the radiation has been given and forgotten. This data certainly gives us pause when offering radiation to very young men with several decades of life expectancy ahead of them, and it also reminds us of the value of follow-up visits.”
“The fact that second cancers arise in the area where radiation was given is not surprising, but the magnitude of the long-term increases is concerning,” added Dr. Marc Garnick, the Gorman Brothers Professor of Medicine at Harvard Medical School and Beth Israel Deaconess Medical Center, and editor in chief of the Harvard Medical School Guide to Prostate Diseases. “There are other common and troublesome urinary side effects of brachytherapy — independent of second cancers — that patients should fully consider before selecting it as a treatment option. This is especially true given the availability of other convenient and similarly effective prostate cancer therapies.”
About the Author

Charlie Schmidt, Editor, Harvard Medical School Annual Report on Prostate Diseases
Charlie Schmidt is an award-winning freelance science writer based in Portland, Maine. In addition to writing for Harvard Health Publishing, Charlie has written for Science magazine, the Journal of the National Cancer Institute, Environmental Health Perspectives, … See Full Bio View all posts by Charlie Schmidt
About the Reviewer

Marc B. Garnick, MD, Editor in Chief, Harvard Medical School Annual Report on Prostate Diseases; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Marc B. Garnick is an internationally renowned expert in medical oncology and urologic cancer. A clinical professor of medicine at Harvard Medical School, he also maintains an active clinical practice at Beth Israel Deaconess Medical … See Full Bio View all posts by Marc B. Garnick, MD

Health care should improve your health, right?

It’s undeniable: modern medicine offers ever-expanding ways to heal and prevent disease. But it’s also true that health care can cause harm. One analysis found that about 6% of health care encounters caused preventable harm, leading to thousands of deaths each year. And it’s not just errors that cause trouble. Highly skilled health care providers can cause harm even when they do everything right.
So, how can you reduce your chances of being harmed? Understanding what you can do to lessen the possibility of harm and what’s beyond your control are good first steps.
Whatever happened to “first do no harm”?
Fortunately, it remains a central tenet of medical care. Yet our health care system is complex and fragmented. Each year new medications are added to an ever-growing list, and people live longer with more chronic medical conditions than happened in the past. So in one sense, the successes of modern medical care may contribute to the high rate of health care–related harm.
These harms are often due to our complicated system of health care rather than one individual’s mistake. Harm due to substandard or negligent care is known as medical malpractice. Both health care providers and health care systems have important roles to play in preventing harm to patients.
Are there harms that cannot be prevented?
An enormous volume of scientific research teaches the best ways to diagnose, treat, and prevent disease. Yet people can react to treatments in completely unpredictable ways.
For example, a common and standard antibiotic treatment (think penicillin) can cause anaphylaxis, a life-threatening allergic reaction. Fortunately this is rare, but unless you or your doctor know to avoid it due to past side effects, there’s always a small chance of a severe reaction.
Often less dramatic — yet also unpreventable — harms are:
- Medication side effects. Every medicine comes with potential side effects, such as nausea, sleepiness, or rash.
- Misdiagnosis. Because no one has perfect diagnostic skills, even the most skillful health care provider can be wrong. This can result in unnecessary or delayed treatment.
- Inaccurate test results. Just as no health care provider is perfect, no test is either. False-positive results (indicating an abnormality when none is present) and false-negative results (normal results when disease is present) are common in medical practice. These results can lead to unnecessary treatment or false reassurance.
Which harms can be prevented?
Preventable harms can be dramatically reduced. They’re often due to mistakes that can be caught and corrected. Frequently, it takes a combination of things to go wrong for harm to occur.
The “Swiss cheese model” is often applied here: imagine you’re a fly trying to travel through several chunks of Swiss cheese. (I know it’s an odd scenario, but stick with me here.) It’s impossible to fly through the cheese unless the holes line up just so.
Frequently in health care, several factors must line up for an error to sneak through — for example, giving a hospitalized patient a medication to which they are allergic. For that to happen, the wrong drug has to get past the prescribing doctor, the computerized ordering system, the hospital pharmacist, the nurse giving the medication, and the patient. That’s a lot of layers, so most often an error like this will be caught.
What can you do to avoid preventable harms?
Where do you fit in? In these three scenarios, here’s what you can do to avoid preventable harms.
The problem: Taking medicines you no longer need or more medicines than necessary.
It might not seem like a big deal to keep taking a medicine if it isn’t causing any problems. But all medicines can cause side effects that you’d do better to avoid if you can safely stop taking it or reduce the dose. Plus, harmful interactions can occur if another medicine is added to your list.
What you can do: Make sure you know why you need to take each of your medicines. Ask the providers who prescribe each medicine if it is still necessary to take it or if the dose can be safely reduced. Reducing a dose may reduce the risk of side effects and the likelihood of a harmful interaction.
The problem: Taking the wrong medicine or the wrong dose.
What you can do: At your doctors’ visits, take notes or bring a friend or family member to help you remember medicine instructions. Ask whether you can record the medication instructions your doctor gives you. Take a photo of the instructions you’re given in case you lose the written version. Double-check details of your medicine list with your pharmacist. And ask questions if you’re unsure about the medicines recommended to you.
The problem: Wrong site surgery.
Despite efforts to make this a “never error,” surgery on the wrong part of the body still happens.
What you can do: Make sure you and your surgeon agree on what part of your body and which side requires surgery. Most surgeons now mark the site with a special pen before surgery and ask you to confirm the site by adding your initials. (The ink doesn’t come off easily with skin cleaners applied prior to surgery).
Some of these tips require time or resources that aren’t available to everyone: you might not be able to bring another person with you to medical visits or have a recording device. But asking questions — and getting answers you understand — should be routine.
Where does malpractice fit in?
When the topic of health care–related harm comes up, malpractice may be the first thing you think about. Yet, the approximately 10,000 malpractice payments made each year in the US likely represent only a small portion of all harm related to health care.
There are several reasons for this, including:
- Even when negligent or substandard care occurs, it doesn’t always cause major or long-lasting harm that leads to a malpractice claim.
- Many people who could file malpractice suits elect not to, or may not even realize that they’ve experienced negligent care. Past studies suggest that less than 5% of people experiencing harm related to medical care file malpractice claims.
- Increasingly, health care providers and health care systems accept responsibility for preventable harm occurring on their watch, and offer compensation rather than waiting for a legal claim to be filed.
The bottom line
It’s an unfortunate reality that some harms due to health care are inevitable. But there are steps you can take to avoid preventable harm and lessen the chances that the person harmed is you.
About the Author

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Robert H. Shmerling is the former clinical chief of the division of rheumatology at Beth Israel Deaconess Medical Center (BIDMC), and is a current member of the corresponding faculty in medicine at Harvard Medical School. … See Full Bio View all posts by Robert H. Shmerling, MD